I used to travel to Nazret after teaching Bible and four French lessons on a Thursday. Nazret v Adama It was about a hundred kilometre trip. I’d book in at the hotel where I always stayed and after freshening up a bit go to the hospital. There was a wide variety of cases as you would expect in a city of about half a million and draining a fairly densely populated area of about 50 km radius. They did operations through the week. They tended to keep the more difficult ones for me. In that area there were lots of cases of cancer of the oesophagus.

People tended to store their food after harvest and it is thought that mouldy stored grain and then eaten is one of the causes of cancer of the oesophagus. This may have been the cause in this area, but whatever the cause it was common.
There are four common modalities of treatment for cancer and they apply to oesophageal cancer as well.
- Surgery
- This was only available in Addis, and if you didn’t have strings to pull, the wait to get an appointment, much less treatment was 6 months or more.
- Chemotherapy, which was even more difficult to get than radiotherapy.
- A combination of the above, which is difficult if only one option is available.
With surgery alone you can hope to occasionally cure, but more often to palliate and extend life at least a bit. Life is precious! People tended to be poor, unprepared to go to the capital, which was expensive and where they knew nobody. They also tended to present late, have difficulty in swallowing and to have already lost a lot of weight.

Foreseeable difficulties – You usually have to do two incisions – in the abdomen and in the chest, and occasionally one in the neck also. Chest anaesthesia has a few added difficulties from other general anaesthetics. Physiotherapy to help with postoperative breathing is necessary; there was no available intravenous parenteral nutrition – ie they had to be fed directly into their gut. Post operatively you didn’t wan them to eat until you were sure that there was not a leak at your joins. Blood transfusion was possible but had to be kept to a minimum.
Possible positives – patients were stoical and used to bearing pain; they knew that if nothing was done they’d soon be dead; my doctor friend was very committed to making it work, and the nurses saw it as a challenge.
There are several ways to replace an oesophagus. Unlike abdominal gut there isn’t a great length of oesophagus and so it has to be replaced with some other living tissue, not just an area cut out and joined. The replacement could be a) mobilised stomach, b) small bowel, c) a piece of large intestine, whatever you used the blood supply needed to remain intact. The choice depends on different circumstances and I’ve used all three replacements but most commonly we mobilised the stomach and used that.
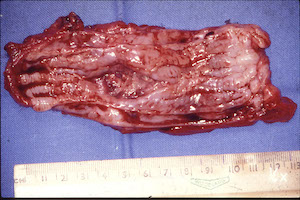
We had no TPN (total parenteral nutrition) so we used feeding jejunostomies ie a tube going through the abdominal wall to the high small bowel. The operation took about 4 hours. One patient was going to die after about a week and requested to be discharged in order to die at home. All the others were discharged home eating, and I don’t know many were cured but they were given a new lease of life.
Telephone; telegram; tell a woman; tell an Ethiopian. They kept coming, so I presume a significant number were satisfied.