Over the years the available investigations for head injuries has increased markedly . In 1962 my very first term as an intern placed me in both a general and a neurosurgical surgical roster. Sitting in bed 6 in bay 1 of the third floor general and neurosurgical ward was a young man who had broken his neck playing Australian Rules Football in High School. It had gone both unnoticed and untreated until he had begun to be paralysed. Before I came on the ward he had been operated on and the tracture fixed, but he was still unable to reach the tasty food which his family brought for him. I especially remember the grapes. I made a deal with him that every time I went past I’d give him some, provided that I got a share. We remained good friends until he died many years later. I assisted in some neurosurgical procedures at that time but never got to do one.
There were no CAT scans or MRIs. As far as trauma cases were concerned there were only plain x-rays, which examined the box (the skull) but not the jewel inside (the brain), and clinical assessments. Regular frequent observations were done on blood pressure, respiratory rate, pupil size and reaction to light, and response to verbal or painful stimulation. Decisions had to be made on these.
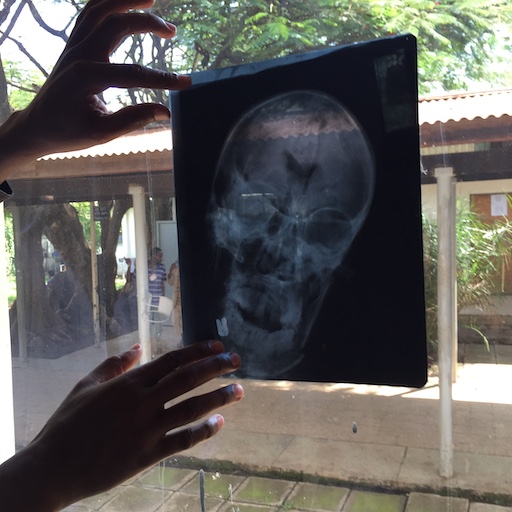
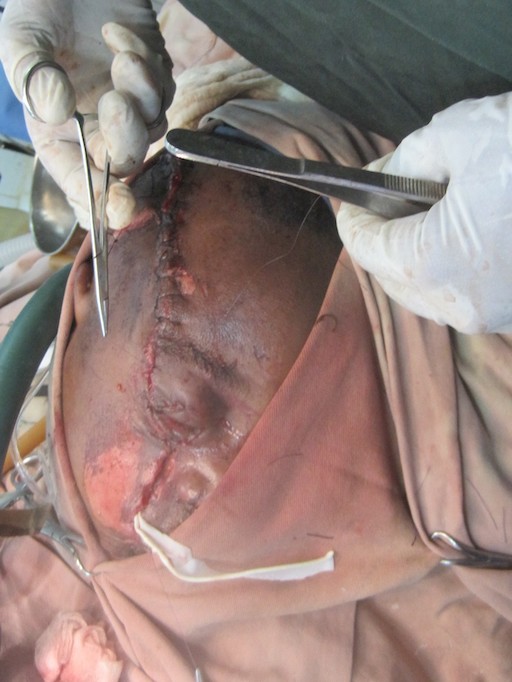
In Ethiopia all my clinical life I had to deal with this level of patient work up for traumatic neurosurgical cases. So I had my share of burr holes, depressed fractures, compound brain injuries etc. In my first stay in the late 60s – early 70s I worked at a place where the farmers used an about 30cm long tool with a narrow (about 8cm wide) hoe like metal end to dig the ground. In anger it would, if necessary, be applied to your enemy’s head. A flap of skin, skull and brain would be raised up. The recipient would often not even lose consciousness but, something had to be done.

In my years teaching at University the young surgeons who came to work with me had little experience of neurosurgery, so I had to work with them, until they gained confidence. There was a neurosurgical unit at the main teaching hospital, which looked after the operative neurosurgical cases. Vehicular traffic had become much more frequent. The accident rate was high. The population had increased from 30 million when we first went to over 100 million so there was increased interpersonal trauma. We had on the average 5 serious traumatic head injuries per week. The common causes of severe trauma there were : –
- Motor vehicles, very often motor bikes.
- Machetes, these had replaced the little hoes of former years, as tools of violence.
- Mango trees. Kids climbing to get mangos would fall on their heads.
- Stones, either applied directly or thrown. Having watched grazing animals as kids had made them accurate at throwing stones to limit the wandering of the animals.
We did some burr holes or craniotomies for bleeds under tension. The majority, however, were for depressed fractures either closed or compound.
It was difficult to get regular observations done, and sometimes they were written up hours in advance so that workers could get a good sleep. Sometimes if recovery wasn’t rapid people. either relatives or nursing staff. would try to send them home and let them take their chances. Many with very low Glascow coma scores on arrival didn’t survive but most did.