Some of the photos below you may find disturbing. Do Not click the READ MORE sign if you are squeamish. They are all medical photos.
Category: Uncategorized

In down country Ethiopia we used to say that in interpersonal trauma the rich – shot each other; the middle class knifed each other; the poor speared each other. We saw many other cases injured with digging hoes, machetes, stones etc, but the case for today was a spearing in the late 1960’s.
A young man had been speared about 4 days previously. They had kept him at home I suspect because they thought he would die. It was an intra-family dispute and they didn’t report it to the police as they understood the reason for the fight and didn’t want the one who wielded the spear imprisoned. He was family and families sometimes fight!
The spear went in his back on the left side and was protruding out of his left upper abdomen. He was not shocked, he was not infected, he was obviously in need of treatment – so no doubt he would have all lots of imaging today but all we had was an old ex-army X-ray machine. We did all the basic things; there was an urgency but not a frantic one so, after an IV was inserted and antibiotics given, he had a thorough clinical assessment, blood was taken and two relatives were sought to give blood. He was taken to the operating room and after the double lumen tube was inserted the spear was removed. (I had to give my own anaesthetics, but fortunately had before training as a surgeon done a bit of anaesthetics and in my surgical training done some thoracic surgery.) I don’t remember the surgery well except that surprisingly little damage had been done to anything. He ended up with an UWSD chest tube in place and a laparotomy scar. He did very well, got on well with the other men in the ward, and was doing extremely well. His chest was good; he didn’t have any unexpected abdominal findings; there were no signs of deep vein thrombosis. On the fourth postoperative day he was laughing and joking with the other chaps, sat up, still laughing, and fell back dead.
I know of only 3 things which cause people to die like that post-operatively. A massive embolus, a massive heart attack and a cerebral incident, a massive stroke. He was young and healthy and I’m sure had an embolus. We didn’t have any anti-coagulants in the hospital so we couldn’t use prophylactic doses against clots. At any rate we saw very few deep vein thromboses, which we of course had to pick up with clinical testing as we had no ultrasound, and often there is no tenderness in emboli which give off massive clot emboli.
At any rate he was instantly dead in a ward in our general hospital, about 500 metres from our operating room which was in the leprosy hospital. Tragedies happen.
Barry Hicks
Diaphragm Injuries

Over the years I have seen a number of diaphragm injuries. Four come to mind as very interestingly different.
- While I was doing a lot of chest surgery, I received an urgent call to come to the OR, where a an obstetrician friend was doing a Caesarian Section. The patient had been in a car accident a couple of years before, and had gone through pregnancy well until when on the operating table, having been given a dose of scoline her left chest became dull and the anaesthetist had to struggle to keep her oxygenated. She had a rapid LSCS making it much easier for the anaesthetist. You could hear bowel sounds in the chest, so with her accident story, we diagnosed delayed rupture of the diaphragm, probably by the rupture of her incomplete tear with the twitches caused by the scoline. She was repositioned and her diaphragm repaired. She and her baby did well.
- A man had been caught between a backing utility and a bench several years before. He was referred to me with a large AAA and a ruptured diaphragm. At the time he had been investigated and no problems found. After work up, and postulating that his prior accident had probably damaged his aortic wall allowing his aneurysm to develop, and that its size had caused an incompletely ruptured diaphragm to completely tear, he was operated on. We repaired both problems at the same time. Obviously this time the diaphragm was repaired from below.
- A grossly obese woman unwisely sat on a glass table. She had a stab wound in her right back, and was operated on by a general surgeon who at laparotomy found a little blood but no other problem and closed the abdomen. She survived but was not well. They did a chest X-ray and found a mass in her right lower chest. I was asked to see her and after investigation explored her right chest finding a complete cut across her diaphragm with the liver totally in the chest. With it repaired she made a rapid recovery.
- The fourth case was seen when one day I made one of my weekly trips to Nazret Hospital when living in Addis Ababa. There was a man who had been stabbed in the back of his right chest. There was an UWSD in place to treat the pneumothorax. He had no abdominal signs or symptoms. But no one had noticed that there was bile coming out the drain! I explored his chest and found about a 5cm laceration in his diaphragm and a considerable laceration into the bare area on the top of his liver. I repaired both liver and diaphragm through the chest. He did well.
Being a surgeon is interesting!
Barry Hicks

I wish that I had had better investigative equipment. I wish that I had had more energy and time to write things up on the spot. As we all know you cannot relive the past. So in my old age I dwell among memories. Some of them very special memories. And that includes this little girl.
She presented short of breath with a high fever, a very tender neck and looking into her mouth you could see a big retropharyngeal bulge, which meant we knew why she had her temperature and was having difficulty in breathing but that bulge was abnormal in a kid of that age in my experience. The X-Ray quality was terrible. We did not have CT scanning or even a decent viewing box in the wards. The following picture shows how we looked at films.

We tried for a soft tissue lateral film and a lateral bone film.

Please don’t be too critical of the films! In the upper soft tissue film you can see how far the air tube is away from the cervical spine. In the lower bony film you can see two bodies which look abnormal.
Where we were, you did something or let nature take its course! Your decision may have been very different from mine but we
- Decided that it probably wasn’t TB and started her on high dose antibiotic.
- With oxygenation and gentle sedation I did a tracheostomy under local anaesthetic.
- We aspirated a huge amount of pus through a large needle through the mouth when she was fully anaesthetized with the trachy in place. This was sent for mcs but had to go to a private lab outside the hospital.
- Made a POP encircling her forehead, strengthened a strip down the back of her neck and encircled the chest.
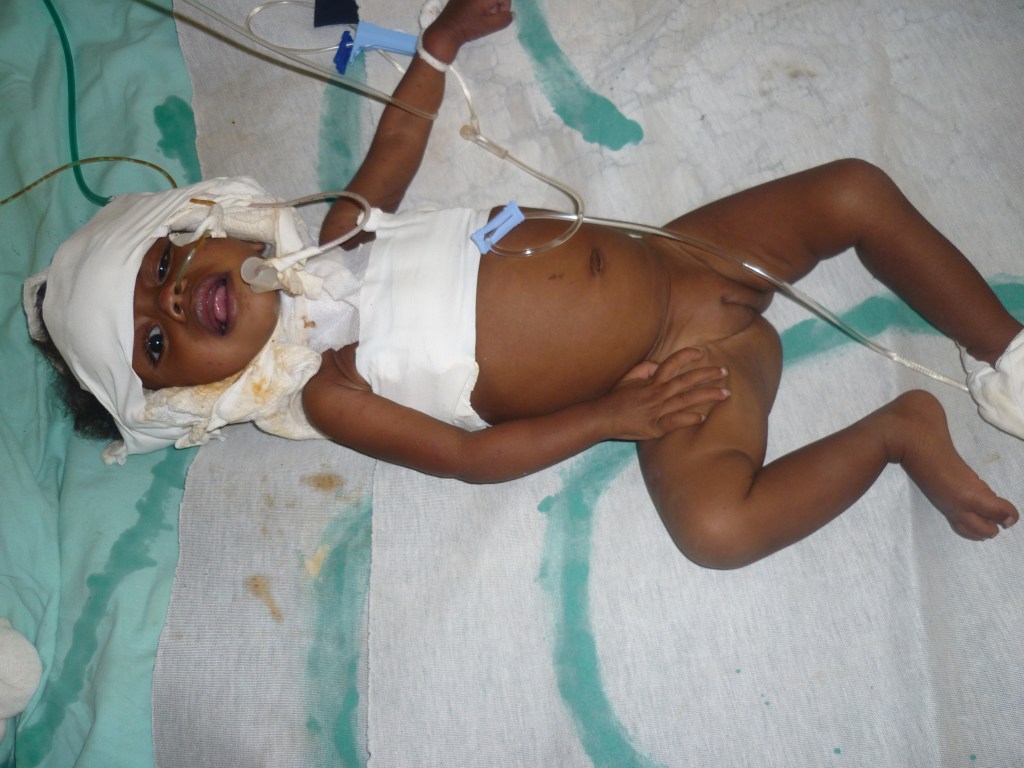
It was not TB but sensitive to our antibiotics. She was on this treatment for 6 weeks, except that her trachy was removed after several weeks when her temperature was down, and by testing she could breath around the tube comfortably.
Either inspite of us or because of us – she got better and went home after about 10 weeks. She wasn’t always happy to have a photograph taken!



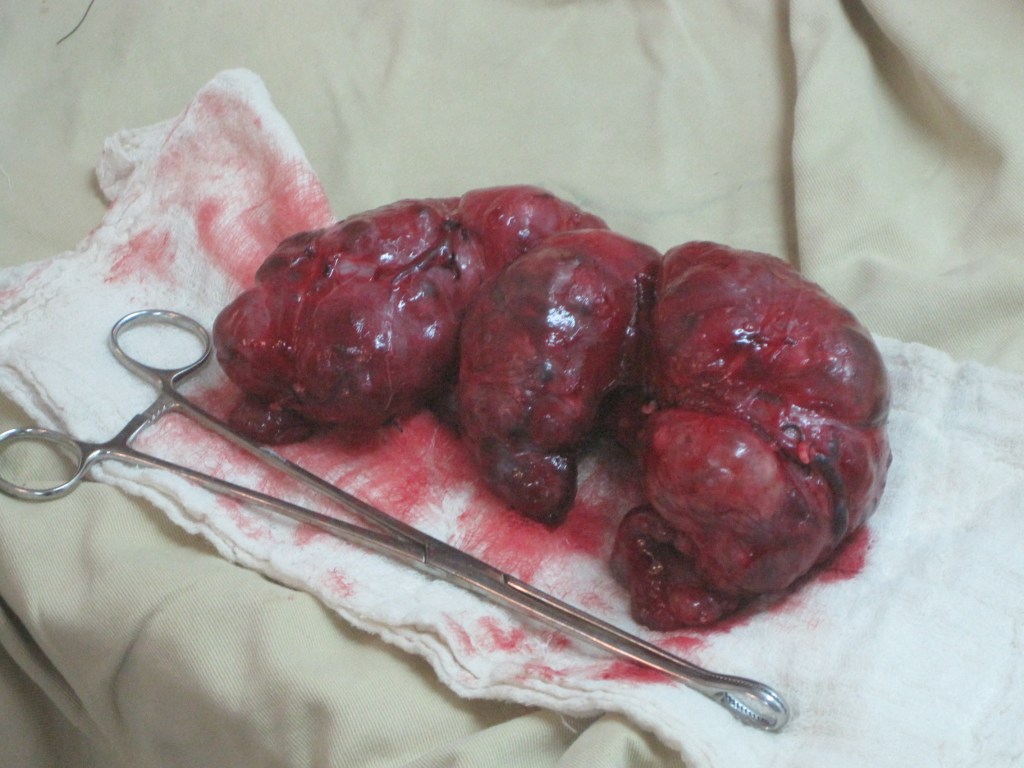




Barry Hicks
Air in the wrong places
Quite an ‘airy experience.



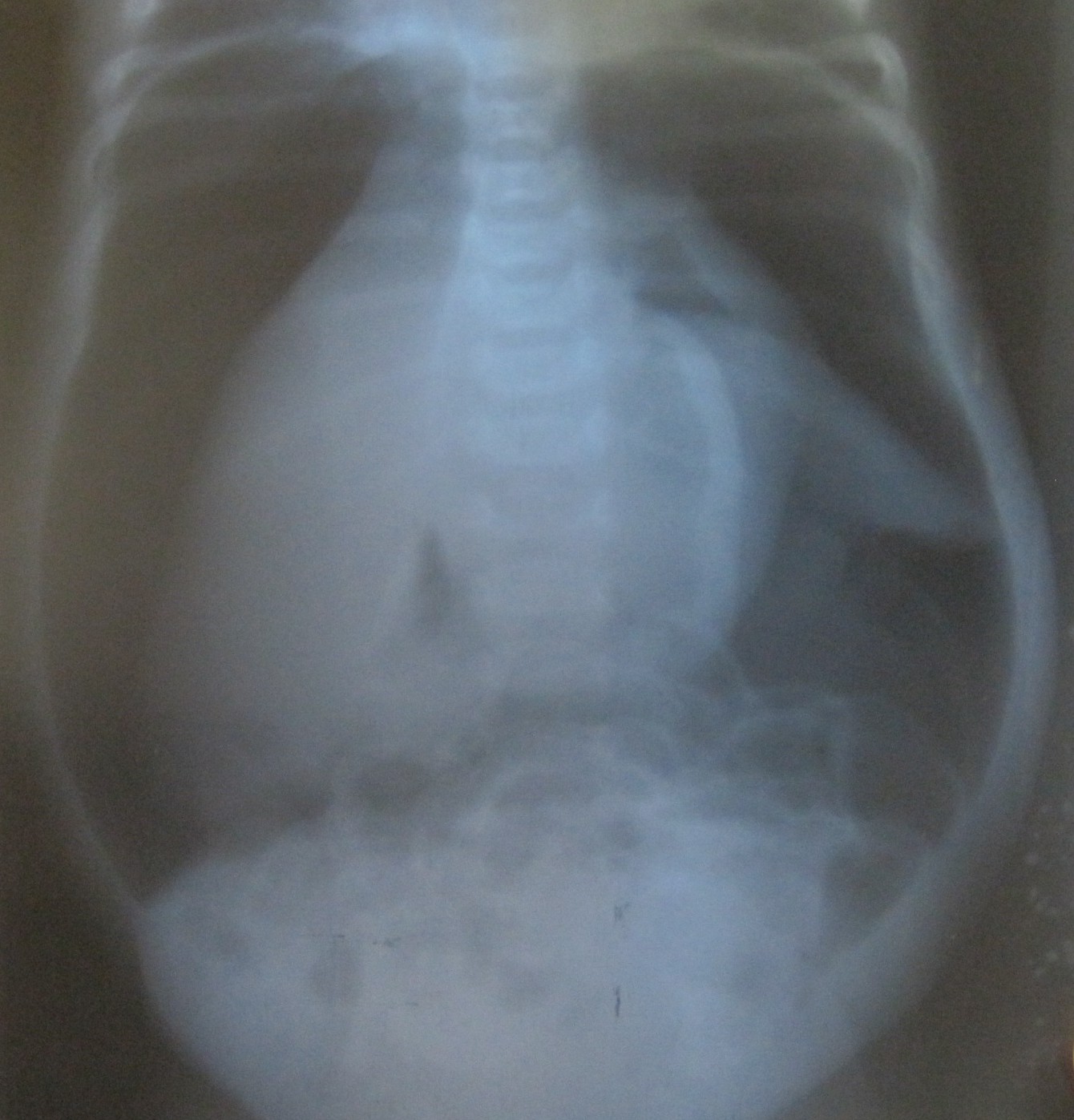
Barry Hicks
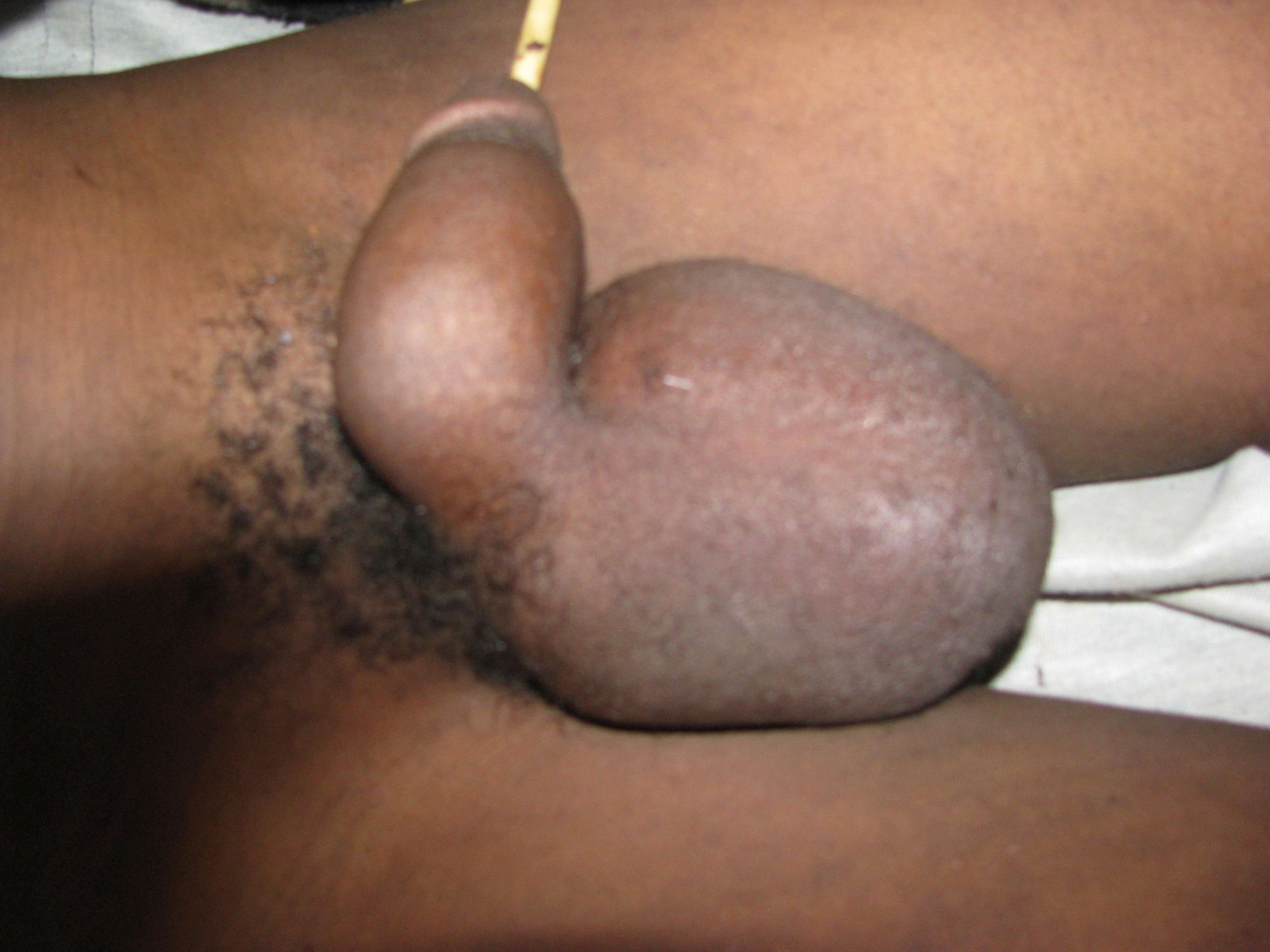
African Limb tumours



I’m not sure that I was ever really fit to be registered as a medical practitioner. In our junior resident’s year we were supposed to be placed under a variety of different specialties. As I remember I was only in three departments. Initially I did a surgical and a medical term each of three months (this was a basic requirement). Then I did a one months spell in the anaesthetic department which became a six months term. After one month I was made a temporary, maybe unofficial, and I’m sure in these days what would be illegal, acting anaesthetic registrar. This was very good for my future overseas time where, as a surgeon, I usually didn’t have an anaesthetist to work with me. The head of the department was either very lazy or very keen to see me get experience. Even on his private lists he would come and see the patient until they were asleep and then I would do the rest until he saw the awakening patient in recovery. I did the night on call duties alone and thus got experience with a great variety of emergency situations, which served me well in my later experience. I used to be amused when my first year contemporaries would ask the anaesthetic department for help in doing things, and then found me there as the one sent to fix the situation. Seriously thank God nothing went wrong.
At the end of that year I was invited to be an anaesthetic trainee, but declined. In my second year out I was in general practice and gave quite a few anaesthetics, both for other GP’s and for a few of the surgeons who were in the area. Fully trained anaesthetists were in short supply in those times even in the major cities.
In the intervening years after that, as I trained as a surgeon, until I arrived in Ethiopia in the late 60’s I didn’t have to think about the head end of the bed!
Until about 2009, when I started working in University hospitals in Ethiopia, I rarely worked with a properly trained anaesthetic doctor. Thus I had to work out a system of how to manage two responsibilities at once.
Where I was initially we had to be careful how much oxygen we used as it was all cylinder oxygen which had to be brought from the capital 250 km away, and our budget was tight. Ether and ethyl chloride were cheap and plentiful. Succylmethoneum (scolinej, as a dried powder, was also plentiful. We had flaxedil and curare as longer term relaxants and an EMO machine for using a measured percentage of continuously supplied ether. Ether, as well as having hypnotic and analgesic properties, is a muscle relaxant. Ketamine was just being developed around then. We had a small stock of Pentothal.
Thus I developed a few principal concepts; –
Use Local anaesthetic if you safely can. LAs are very useful for spirals, cordals, blocks or by infiltration. They were specially useful in Leprosy patients with depressed sensation in many areas.


I have done Caesarean sections under LA. The pain problem comes when placing the hand into the pelvis to get the head freed. Apart from the discomfort of that, by using a larger volume of dilute LA, it is possible.
After a while, for Caesarean Sections, I usually chose this other way. Having everything carefully set up with nurse having prepared the site for surgery and having draped the patient while I was pre-oxygenating her, I put the lady to sleep using Pentothal and scoline to intubate, then I hooked up the EMO Machine on 0% ether. I then rushed out had alcohol poured over my hands, dressed rapidly without scrubbing and began to operate. The reason to do things this way was so that no respiratory depressant nor paralysing drugs crossed the placenta to the baby. Time from the pouring of alcohol on my hands, until the baby was out was about 6-7 minutes. After that ether was added in the EMO machine for the remainder of the operation.
Ether in the lungs rarely makes people vomit. Ether in the stomach is nauseating.
In later years ketamine was very useful. Ketamine was being developed about that time. Its nasty nightmarish effects didn’t seem to worry small patients but in adults it needed to be covered by something like Valium.
Later ECG machines, pulse oximeters, automatic blood pressure machines helped me a lot, as after stabilising the patient and becoming the surgeon the anaesthetic end was monitored but by an untrained person. Well I trained them somewhat, and later one of them gave me an anaesthetic.
As I remember Maurice King, in a book about Anaesthesia in Developing Countries, wrote that a piece of string is an important part of anaesthetic equipment. Its purpose is to tie the anaesthetist to the machine to stop him wandering away. In one of my stints overseas we had a young Eastern European trained anaesthetic nurse attached to the hospital. I came into the operating room one day to find him looking out the window. His patient was dead and he was oblivious to the fact. We managed to resuscitate the patient. I had several other terrifying experiences with him, so reverted to doing my own anaesthetics and letting him watch. He didn’t want to listen to me. He was understandably offended but I have no regrets for doing so.

In my later years there were almost always either nurse anaesthetists or doctor anaesthesiologists. In that period, I had two interesting experiences, one very sad, and one to me amusing.
A nurse anaesthetist was intubating a patient while I was scrubbed waiting to start operating. It was obvious that the tube was in his oesophagus. The nurse absolutely refused to listen to me. I called the Ethiopian Head of the Surgical department in the next operating room. The nurse also refused to listen to him. I did not have a position with authority in that hospital, so was unable to insist and just take over the anaesthetic. The patient died.
The second occurred just as I was retiring. The head of anaesthetics came to me with a hernia which I agreed to repair for him. In the next breath he said to me please give my anaesthetic yourself, I don’t trust any of them!” I did it for him under local anaesthetic!
Barry Hicks
Alternative medicine

Working in Africa you were in competition with other forms of ‘medical practice’. There were witch doctors who sometimes caused us great difficulties. One case that I remember very clearly was a pregnant woman at term who presented in severe shock and bleeding heavily from a placenta praevia. After urgent resuscitation with IV saline as we waited for blood for transfusion her haemoglobin when checked was 3Gm/100mls, about 25% of normal. I have no idea of what her haemoglobin was before she started to bleed but suspect that it was low or she would have been dead. We were very short of blood and there was no blood bank in the area and, using the 2 units available, I quickly did a Caesarean. (She was nowhere nearly fully dilated.) The baby was dead. She survived.
As a first choice she had gone to the witch doctor who sacrificed a goat which she provided. He got the meat, she had to drink the blood to appease the evil spirit causing the problem! It hadn’t helped.
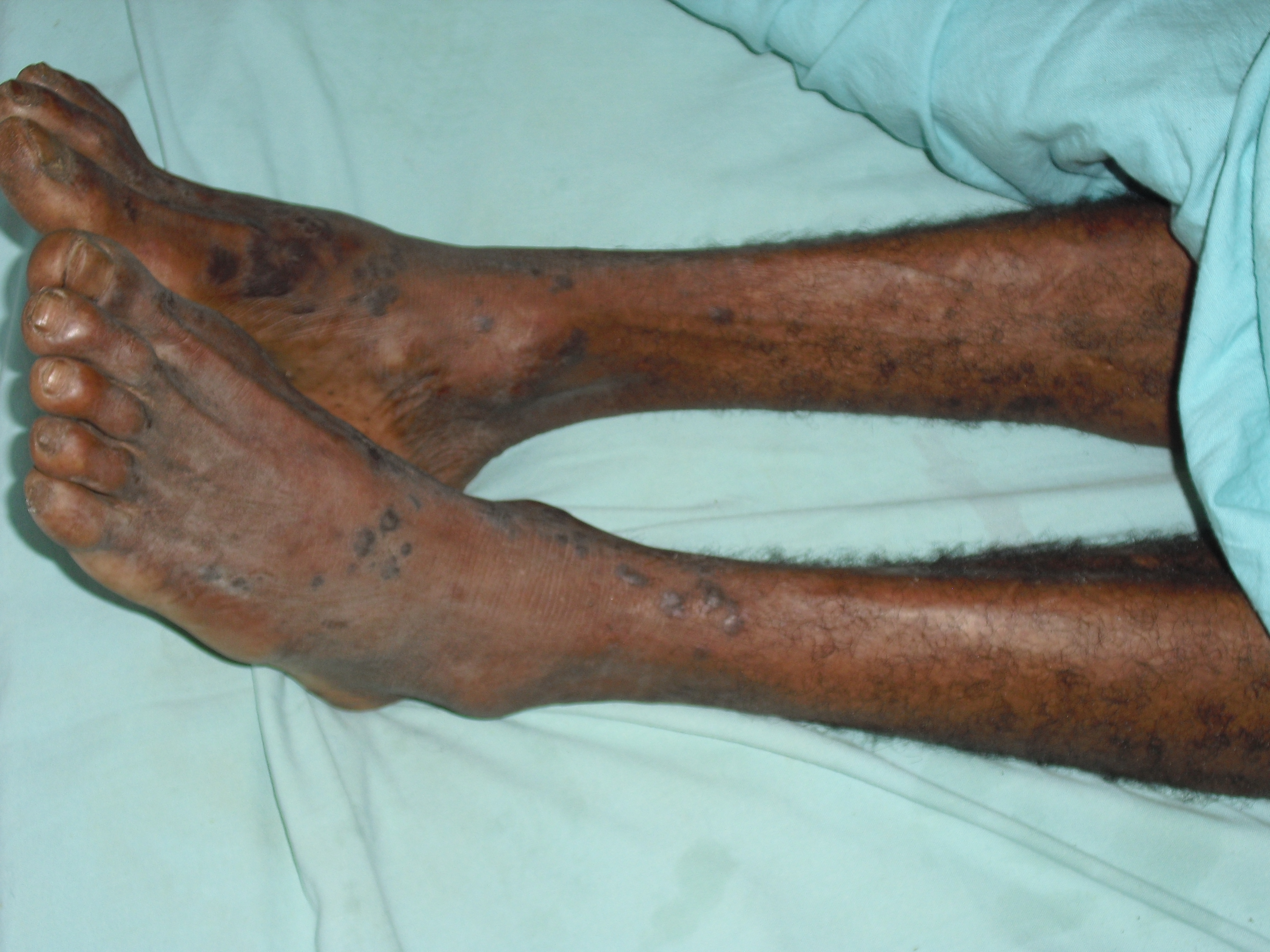
Then there were local healers. I have no doubt that they often did good. A high infant and maternal mortality in the country is a warning that a better system is necessary. But where I mostly met with their failure was in their treatment of fractures. Their major approach was to use external fixation with strips of bamboo tied together very tightly with string. They didn’t have Xrays; they didn’t understand the practice of fixing the joints above and below; they didn’t know how to assess the potential excessive tightness of their fixation with possible nerve, vascular and necrotic problems. They surprisingly didn’t seem to have learned that fractures swell in the early stage of the healing process. We have been ingrained with the 5P principle, watch for – Pain, Pallor, Pulses, Paraesthesia, Paralysis. They do not understand this. They didn’t understand early mobilisation. Therefore we faced initially necrosis with gangrene +/- infection. Then stumps where the limb had dropped off, contracted joints, extreme sepsis etc.
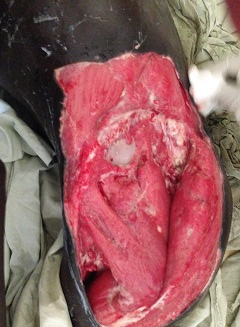
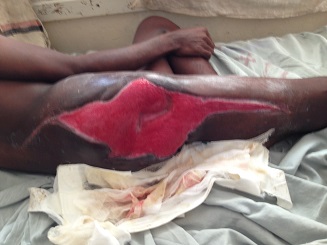
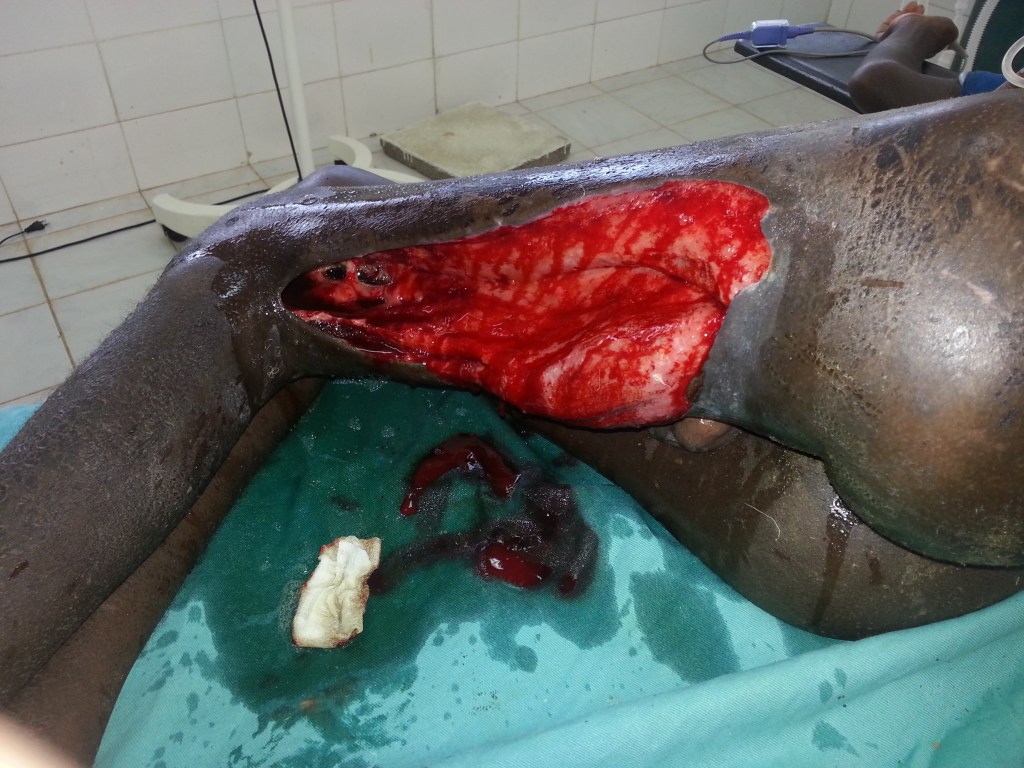
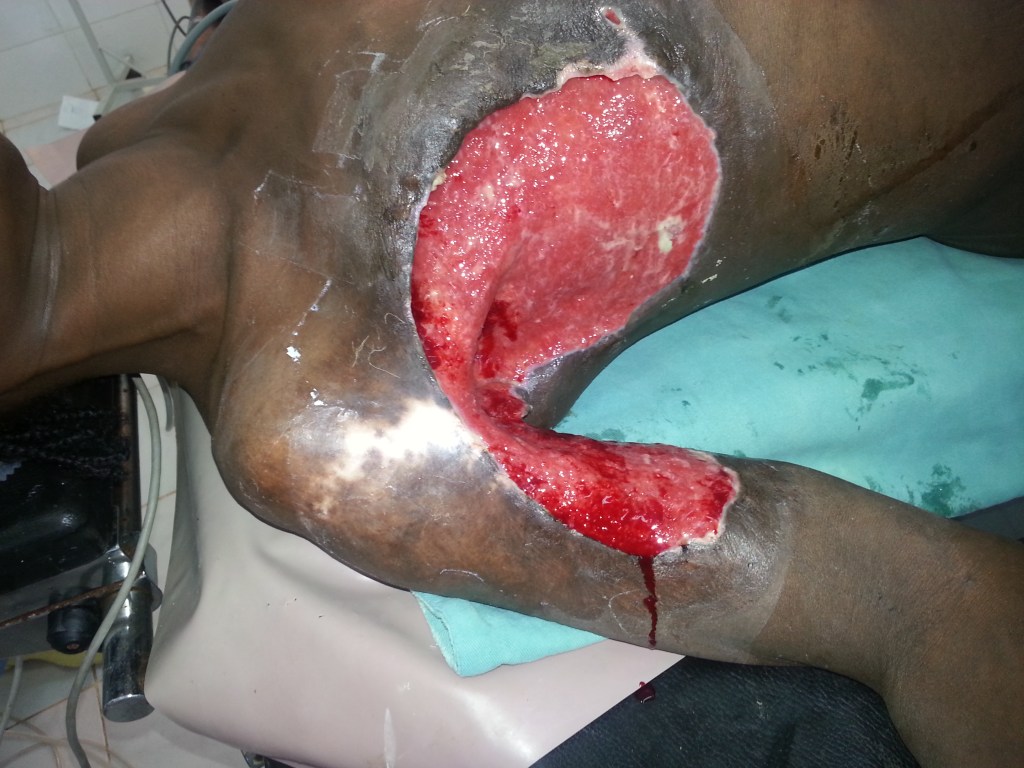
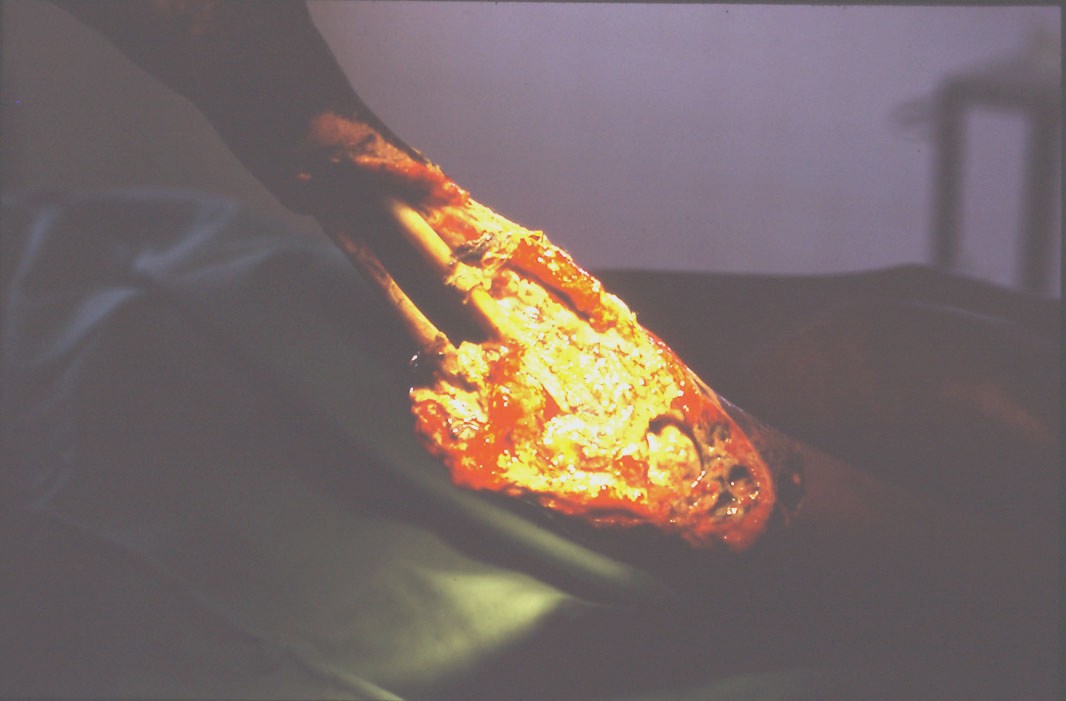
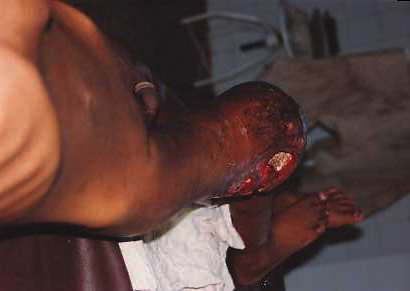
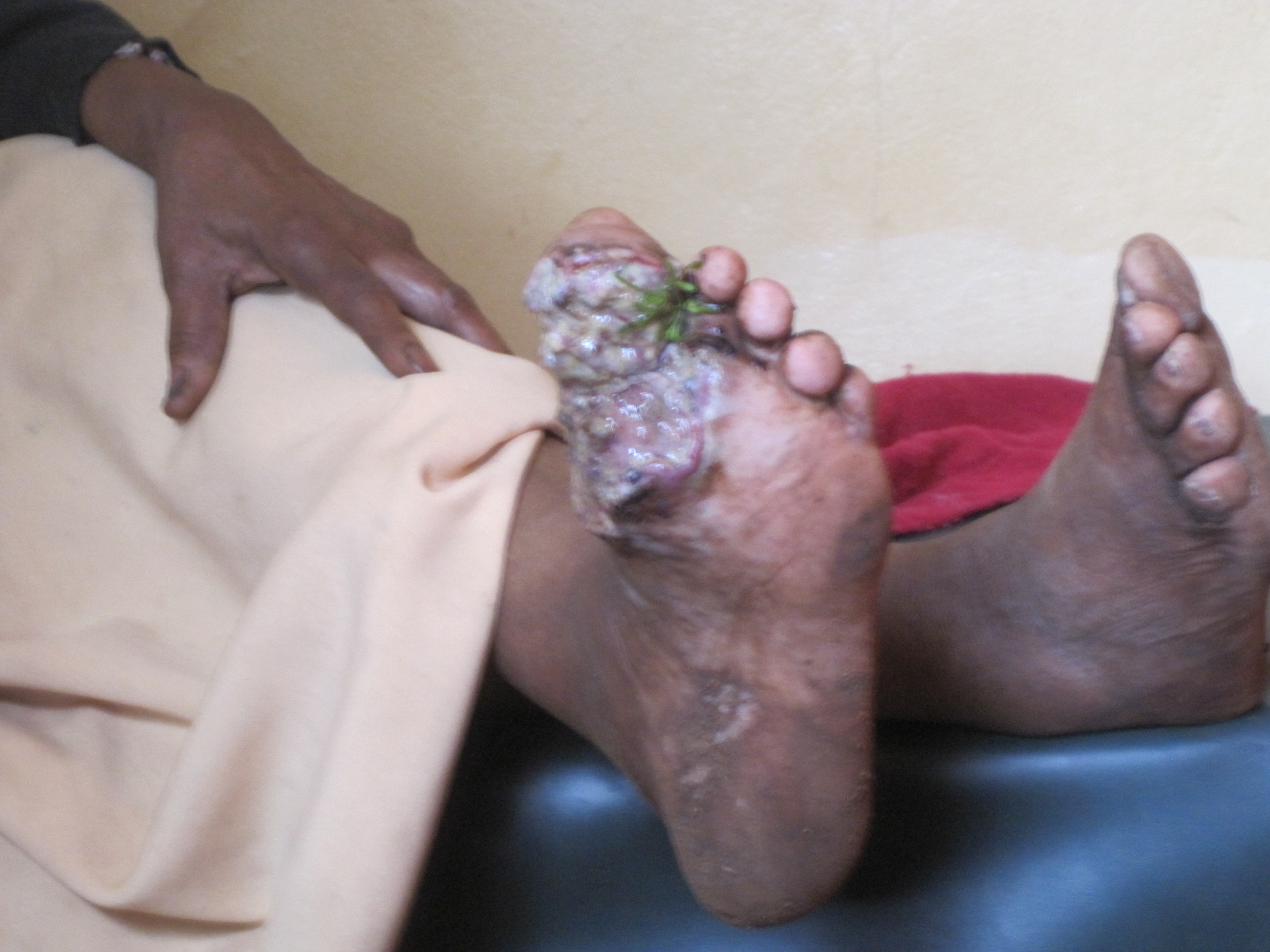
Amputations performed, because of infections, usually had to be of the guillotine type with refashioning when the situation was better controlled. Occasionally on examination of the amputated dead limb we could not find evidence of a fracture. I will show you a few as they presented. Some of the pictures are a bit nasty. It was rare not to have one or more in the ward every week.
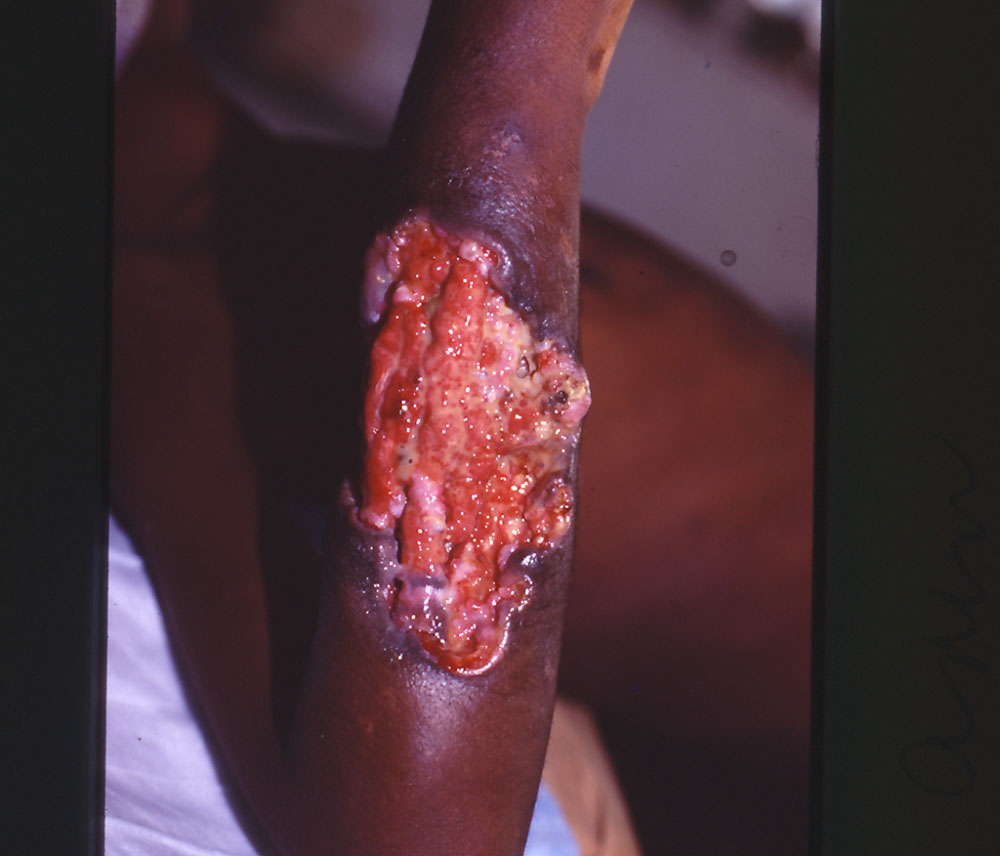
I have seen a ‘spontaneous’ colostomy in a strangulated hernia which presented after days of pain. But even more unusual, shortly after that I had 3 cases of lumbar colostomies in children. One was in a boy who fell onto a sharp stick which went into his right lumbar area. Faeces began to discharge immediately but he lived hours away in an area without roads and his parents were very poor. He lived and after 3 months they had enough money to travel to our hospital. By that time he had developed a huge ulcer as seen in the photo below.